Shalini Malhotra* and Faiz Zaman
Consultant, Department of Obstetrics and Gynaecology, Al Qassimi Women & Children Hospital, Sharjah
*Corresponding author: Malhotra S, Consultant, Department of Obstetrics and Gynaecology, Al Qassimi Women & Children Hospital, Sharjah
Introduction
Uterine rupture is a serious obstetric emergency causing life-threatening situations for the pregnant lady and her fetus needing emergency treatment. While in the olden days, these were due to neglected labor, it has been noticed that most are due to giving way to previous surgery scars on the uterus. A retrospective study reviewing singletons with uterine rupture in a Taiwanese tertiary obstetric center over a 15-year period suggested the overall uterine rupture rate was 3.8 per 10,000 deliveries, with over 59 % being them being through a non-cesarean scar (non-CS ruptures) most commonly, previous laparoscopy myomectomy scars [1]. The scars of the previous myomectomy have been associated with rupture in the third trimester without uterine contractions, particularly between 28-36 weeks which is what makes them even more dangerous.
This case aims to bring to light the silent rupture of a previous myomectomy scar at around 30 weeks gestation with a good outcome.
Case Report
Mrs. F, a 40-year-old lady, pregnant for the second time after a previous spontaneous miscarriage, attended an emergency on 5/5/19 at 27 + 5 weeks gestation with pain abdomen. She was in good condition with safe ongoing pregnancy and thus was discharged from emergency after requesting a urine microscopy check. No infection.
Over 5 years back she had undergone a laparoscopy myomectomy in Egypt with the removal of five fibroids, followed by a hysteroscopy, 4 months after which she was advised to get pregnant. She was on daily Injection of enoxaparin.
She again attended an emergency on 23/5/19 at about 3 am giving a history of pain abdomen, when she was 30 weeks gestation. With stable vitals, she had no significant findings on abdominal examination and the CTG was normal too. She thus refused to get admitted for observation. However, she reattended an emergency at around 9 am with an increased pain abdomen, with an inability to pass urine. She was perceiving normal fetal movements. She has immediate assessment and catheterization with 120 ml of urine drained. On abdominal examination, tenderness noted all over the abdomen through fundal height made out entirely and CTG was normal. USG obstetric revealed a well-grown fetus with normal liquor.
On abdominal ultrasound done by the radiologist after an hour, to look for a cause for acute abdomen, moderate ascites noted with gravid uterus seen. The surgeons were called in to analyze the possible cause of acute abdomen with as cited moderate and with suspicion of appendicular rupture/lump, diagnostic laparoscopy was planned.
On laparoscopy, hemoperitoneum has seen, approximately 1.2 liters, and thus decision for laparotomy taken immediately jointly by Surgeons and Obstetricians as a source of bleeding could not be found due to clots filling the pelvis. On midline laparotomy, major hemoperitoneum seen. Spleen, liver visualized with difficulty but normal. Upon evaluation of uterus and adnexa, a vertical rent noted in the posterior uterine wall, 5 cm long with a bag of membranes seen through it. Both sides tubes and ovaries visualized with difficulty but noted normal. The immediate decision for delivery of the fetus with the repair of the uterus taken and the husband was briefed all through the surgery about the course.
Healthy baby delivered by cesarean section and resuscitated by pediatricians and shifted to NICU. Uterus cleaned and rent repaired in three layers. No other defect noted. after thorough abdominal lavage and inserting intra-abdominal drains, the abdomen closed in layers and the patient shifted to ICU after 2 liters blood loss estimated and 3 units blood and 4 FFP transfused. Post-op, she was observed in ICU for 24 hours and recovered well and was discharged well on day 10 after wound healing was good. She was seen after 4 weeks at the postnatal clinic and was found to be recovering well, breastfeeding her baby well and was advised to avoid pregnancy for at least 2 years and ensure early booking in next pregnancy with timed delivery by cesarean section around 34-36 weeks (Figures 1 and 2).
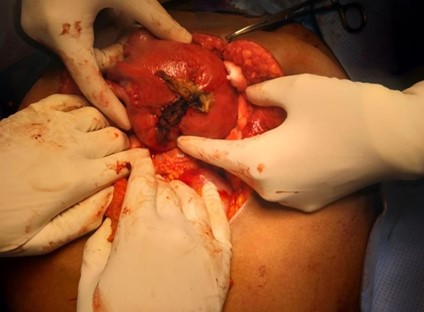
Figure 1: Post repair rupture site with surgical
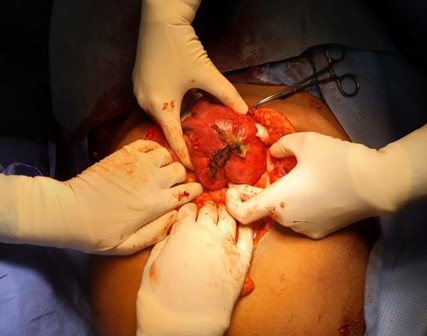
Figure 2: Site of rupture in the posterior wall, the upper part near the fundus
Discussion
The occurrence of myomas are frequent – 20 - 40 % in women of reproductive age [2]. This can be attributed to more imaging and delayed childbearing in women. Apart from the delayed age of conception as a single most important factor affecting spontaneous conception. there are many other reasons for infertility too with uterine disorders like myomas playing a significant role. Myomas are present in 27% of infertile women [3,4]. Even with it established that usually, submucosal myomas affect fertility maximum with serosal myomas causing minimal effect most infertile women are subjected to myomectomy. While the effectiveness and safety of the subsequent pregnancy are still uncertain, in women having the previous myomectomy, many women are subject to it.
The rate of myomectomy in women of reproductive age group is increasingly being opted to be done by minimally invasive technique- laparoscopy or robotic. The skill of the surgeon is essential to ensure good repair of the myoma bed to leave a strong scar for the future. Pregnancies in these women after myomectomy thus becomes challenging for their obstetricians, especially as various studies have shown myomectomy scars 0.6 % are at a greater risk of rupture during pregnancy as compared to cesarean scar rupture which is approximately 0.3% or septoplasty (0.02 %) scars. The risk of rupture is present whether done by laparoscopy (1.2 % ) or laparotomy (0.4 % ) (meta-analysis) [5].
The main findings of most studies related to scar rupture, concluded as follows:
- patients with a history of endoscopic uterine surgery should be aware of uterine rupture during pregnancy.
- the time interval from surgery to pregnancy was significantly shorter in the non-CS than in CS ruptures.
- severe bleeding (blood loss > 1500 mL) requiring transfusions was more frequent in women who experienced non-CS compared with CS ruptures; and
- when the uterine rupture occurred, admissions to the neonatal intensive care unit were significantly more frequent in preterm than in term pregnancies. Neonatal morbidity like perinatal hypoxia cerebral palsy and mortality was up to 33 % [6].
There are some suggestions referring to myomectomy to reduce the risk of uterine rupture in a subsequent pregnancy. It seems that the method of sewing the uterine closure is crucial. For example, multilayer uterine stitches, preservation of the endometrial cavity, and avoidance of using electrosurgery to prevent devascularization (to avoid hematoma formation) should be taken into consideration to prevent weakness of the wall of the uterus. Uterine scars differ histologically and biochemically.
The purpose of the myomectomy in a young woman should be well considered. In cases of infertility, removal of the intrauterine lesions is usually necessary to give the patient a chance of pregnancy. At the same time, the risk of uterine rupture is increased. Honest and detailed counseling of women undergoing endoscopic uterine surgery, including the ideal timing of pregnancy after endoscopic uterine interventions, and awareness of obstetric complications to optimize subsequent pregnancy outcomes, is important.
References
- Chao AS, Chang YL, Yang LY, Chao A, Chang WY, et al. (2018) Laparoscopic uterine surgery as a risk factor for uterine rupture during pregnancy. PLoS One 13(5): e0197307.
- Bulletti C, Dez D, Levi Setti PL, Cicinelli E, Polli V, et al. (2004) Myomas, pregnancy outcome, and in vitro fertilization. Ann NY Acad Sci 1034: 84-92.
- Practice Committee of the American Society for Reproductive Medicine in collaboration with Society of Reproductive Surgeons (2008) Myomas and reproductive function. Fertil Steril 90(5 Suppl): S125-130.
- Borgfeldt C, Andolf E (2000) Transvaginal ultrasonographic findings in the uterus and the endometrium: low prevalence of leiomyoma in a random sample of women age 25-40 years. Acta Obstet Gynecol Scand 79(3): 202-207.
- Rees M (2018) Case reports in women’s health. 19.
- Kim HS, Oh SY, Choi SJ, Park HS, Cho GJ, et al. (2016) Uterine rupture in pregnancies following myomectomy: A multicenter case series. Obstet gynaecol sci 59(6): 454-462.



