Honglian Xia1, Zhongwei Guo1, Haokai Zhu2, Lijuan Wang1*
1Tongde Hospital of Zhejiang Province, Zhejiang Mental Health Center, Hangzhou, Zhejiang 310012, China
2The Second Clinical Medical College, Zhejiang Chinese Medical University, Zhejiang 310000, China
*Corresponding Author: Lijuan Wang, Tongde Hospital of Zhejiang Province, Zhejiang Mental Health Center, Hangzhou, Zhejiang 310012, China.
Abstract
The Behavioral and psychiatric symptoms of dementia (BPSD) seriously affect the quality of life of patients and caregivers. Doll therapy can alleviate the wandering symptoms of dementia, improve sleep quality, and increase the happiness of patients. However, the specific mechanism has not been clarified at present. Doll therapy opens a window for us to study BPSD.
Keywords: BPSD, Doll therapy
Introduction
More than 90 % of dementia patients will have behavioral and psychiatric symptoms of dementia (BPSD), such as anxiety, depression, wandering, sleep disorder, delusion, etc. There are many hypotheses about BPSD. Kovach et al. [1] considered that BPSD might represent a patient’s attempt to express physical or emotional distress in response to unmet needs. Brittain et al. [2] proposed that BPSD might indicate that the patient perceives a threat that needs managing. Doll therapy (DT) is a non- pharmacological intervention, that aims at reducing the level of anxiety and agitation in patients affected by moderate to severe dementia, mostly in nursing homes [3]. Our previous studies have also found that DT can improve the wandering symptoms of dementia patients [4,5], indicating that DT can help dementia patients become calmer and further adapt to the surrounding environment, thus improving wandering. Now, the following two reports may help us understand the inner world of dementia patients more comprehensively than those above.
Case Presentation
Case 1, Chen ××, who was female and 85 years old, had progressive memory loss for more than four years. In the past three months, she had significant behavioral abnormalities. Sometimes she sat on the chair crying or calling her mother, sometimes kept shaking the chair, and sometimes hit herself with her hands. In particular, when eating, she didn't eat, persuasion was useless. She was unwilling to eat or cried while eating. Caregivers were difficult to manage. Psychological comfort and antidepressants had no obvious effect. One day, I walked into the patient with my doll. When she saw the doll I held, she liked it and wanted to hold it. She was very happy and couldn't put it down. She teased the “baby”, kissed and hugged her, and kept saying, "how lovely (Figure 1)." She took a cup and fed water to the “baby” (Figure 2). "It's time to eat. First, feed the baby." She said to the doll. I told her that it was time for the baby to take a nap, you should eat quickly and take a nap with the baby later. She promised to eat as soon as possible to replace me. Then she took a big bite (Figure 3). The whole process was happy, and she truly experienced the happiness of accompanying and raising a “baby” and the sense of responsibility for taking care of children. It is no longer like doing nothing.
Figure 1: Grandma Chen caresses the doll
Figure 2: Grandma Chen fed water to the doll
Figure 3: Grandma Chen ate by herself
Case 2, Wang ××, who was female and 80 years old, had been suffering from dementia for 3 years. For the past half a year, she was unwilling to speak and communicate with others. Also, she was unwilling to go out for a walk or watch TV. She sat alone most of the day with a depressed expression. The caregiver took the patient to the ward for medical help, hoping to improve the depression. When she saw the doll, she loved it very much, and a satisfied smile appeared on her face (Figure 4). One day, she sat on a chair and quietly held her doll. When I walked to her, she saw that my doll was not dressed. She was very worried. I put the doll in front of her. She touched the “baby's” hand and said: was the baby cold? Ask herself and answer herself: it's cold. She caressed the doll lovingly (Figure 5). I put a towel on the table, and she immediately wrapped it up for the baby and said: it won't be cold. Then she smiled happily (Figure 6).
Figure 4: Grandma Wang looked after the doll with a smile on her face.
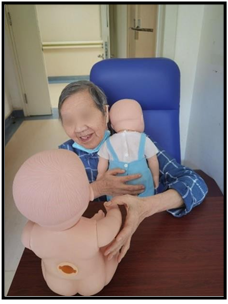
Figure 5: Grandma Wang caressed the doll and said it will be cold without clothes.
Figure 6: Grandma Wang dressed the doll herself and was very happy.
Discussion
At present, there are three hypotheses for the mechanism of DT [6]: Attachment Theory, Transitional Object Theory, and Person- centered Theory. The attachment theory [7] postulates the need for a human being to establish affective bonds when facing unknown situations. The Transitional Object Theory [8] is based on the calming properties that certain objects may have to alleviate and diminish anguish [9,10]. The Person-centered Theory was developed by Carl Rogers in 1961 [11] and places the individual at the centre of care, being supported and trained to be able to collaborate with the decision-making process [12]. The common point of the above theories is that they are patient- centered and need to be loved. However, our observations show that it is the doll centered and the patient releases love. The patient fed and dressed the doll. They are full of love for dolls. After the doll is eaten, the patient can start eating again. The doll is dressed and the patient is happy. In other words, the happiness of patients is based on the happiness of dolls. The observation of patients affected by dementia interacting with the doll shows that they treat the doll as a real baby needing care and hence they might replace their attachment request with caregiving behaviours.
Frequently patients interact with the doll taking care of her needs, reassuring and lulling her.
At present, we cannot truly understand the inner world of dementia patients, the following two materials may give us some enlightenment. One book, named “Grandpa and Lucy”, written for children (Lucy) and families, deals with the onset of behavioral changes in a beloved grandfather who is experiencing dementia [13]. On a warm spring day, Lucy visited Grandpa, who said that today he would like to take her to see the “Princess Butterfly” movie at the local movie theatre. When Lucy pointed out that the time of the movie was wrong, Grandpa began to call Lucy “Miranda” and told her he was certain, becoming outraged. The next day, when Mom and Lucy went to visit Grandpa, Lucy brought a bag of activities and games that she and Grandpa could play. She did not correct him when Grandpa called her “Miranda” and they enjoyed a lovely time looking at old photos and sharing the remembrances of his childhood. This story reminds us that dementia patients felt happy in sharing, but their emotions were fragile. Another inspiration comes from the art therapy of dementia patients [14]. Art therapy enhances self-esteem and improves communication. In our clinical practice, it is often found that dementia patients change clothes of different colours for dolls every day, tidy them up, and then look at the dolls with satisfaction. Use different tableware to feed water to the doll, and then happily say that the baby is full. Then, put the doll quietly in front of you to enjoy. It seems that they are appreciating their works of art and are intoxicated with the realization of their value. Therefore, we speculate that doll therapy provides a way for dementia patients to release love and thus have a sense of self-fulfilling achievement.
Conclusion
DT can improve BPSD and increase the happiness of patients. The mechanism may be derived from Attachment Theory, Transitional Object Theory, and Person-centered Theory. It may also derive from the need to release love and self-realization. Their inner world may be related to past experiences, personality factors, and genetic factors. DT has opened a window for us to understand their inner world. However, we still need to explore what they are thinking.
Informed consent: Informed consent was obtained from the patient to publish this case report.
References
- Kovach CR, Noonan PE, Schlidt AM, Wells T (2005) A model of consequences of need-driven, dementia- compromised behavior. Journal of nursing scholarship: an official publication of Sigma Theta Tau International Honor Society of Nursing. 37(2): 134-140.
- Brittain K, Degnen C, Gibson G, Dickinson C, Robinson L (2017) When walking becomes wandering: representing the fear of the fourth age. Sociology of health & illness. 39(2): 270-284.
- Cai X, Zhou L, Han P, Deng X, Zhu H, et al. (2021) Narrative review: recent advances in doll therapy for Alzheimer’s disease. Annals of palliative medicine. 10(4): 4878-4881.
- Wang L, Zhu H, Xia H, Guo Z (2022) Doll Therapy May Be a Quick Way to Improve the Wandering Symptoms of Dementia: Two Case Reports. Int J Psychiatr Res. 5(2): 1-3.
- Wang L, Song Q, Pan Y, Zhang Z, Zhai C, et al. (2022) Effect of doll therapy on wandering symptoms in patients with dementia: A preliminary clinical observation. J Nurs Educ Pract. 12(9): 33.
- Martín-García A, Corregidor-Sánchez AI, Fernández-Moreno V, Alcántara-Porcuna V, Criado-Álvarez JJ (2022) Effect of Doll Therapy in Behavioral and Psychological Symptoms of Dementia: A Systematic Review. Healthcare (Basel). 10(3): 421.
- Pezzati R, Molteni V, Bani M, Settanta C, Di Maggio MG,et al. (2014) Can Doll Therapy Preserve or Promote Attachment in People with Cognitive, Behavioral, and Emotional Problems? A Pilot Study in Institutionalized Patients with Dementia. Front. Psychol. 5: 342.
- Winnicott DW. Realidad Y Juego. Gedisa; Barcelona, Spain: 1974. Objetos transicionales; pp. 17–45.
- Stephens A, Cheston R, Gleeson K (2013) An Exploration into the Relationships People with Dementia Have with Physical Objects: An Ethnographic Study. Dementia. 12(6): 697–712.
- LoboPrabhu S, Molinari V, Lomax J (2007) The Transitional Object in Dementia: Clinical Implications. Int. J. Appl. Psychoanal. Stud. 4(2): 144–169.
- Rogers CR (1961) The Place of the Person in the New World of the Behavioral Sciences. Pers. Guid. J. 39(6): 442–451.
- Kitwood T (1998) Professional and Moral Development for Care Work: Some Observations on the Process. J. Moral Educ. 27(3): 401–411.
- Parker M (2018) A Review of Grandpa and Lucy: A Story about Love and Dementia. Issues Ment Health Nurs. 1-4.
- Chancellor B, Duncan A, Chatterjee A (2014) Art therapy for Alzheimer's disease and other dementias. J Alzheimers Dis. 39(1): 1-11.








