Rajaa El azzouzi1,2*, Olaya Hamidi1,2, Alain Habimana1,2,Ghita Alami1,2, Bouchra Dani1,2, Malik Boulaadas 1,2
1Department of Maxillofacial Surgery Hospital of Specialities Rabat, Morocco.
2Faculty of Medicine and Pharmacy of Rabat. Mohammed V University in Rabat, Rabat, Morocco.
*Corresponding Author: Rajaa El azzouzi, Department of Maxillofacial Surgery and Stomatology, Hospital of Specialities RABAT; CHU Ibn Sina, Av. Abderrahim Bouabid, Rabat-Morocco.
Abstract
Tuberculosis of the tongue is a very rare event even in areas and countries in which tuberculosis is endemic like Morocco.
The disease can present itself in a variety of clinical appearances, most of which may clinically mimic malignant lingual neoplasms.
We present a case of a 65 years old female patient who presented with the complaint of nonhealing ulcer of lateral border of tongue for 1-month duration which was suspected to be a squamous cell carcinoma on clinical examination. Deep biopsy was taken, histopathological examination revealed that it was tuberculosis. An additional workup was initiated to rule out pulmonary tuberculosis and to search for another localization; revealed the association of lymph node tuberculosis, a phtisiological opinion was sought to start antituberculosis treatment.
TB is a major public health problem in a lot of developing countries with high contagiousness, thereby requiring the early diagnosis and prompt treatment.
Keywords: Tuberculosis, tongue, case report.
Introduction
Tuberculosis is a chronic granulomatous disease, caused by Mycobacterium tuberculosis that can affect various systems of the body, with considerable fatality. Typically affecting the pulmonary system and, rarely, other body organs. Primary tuberculosis of the oral cavity is a very rare condition. In most cases, it is secondary to pulmonary tuberculosis.
In Third World countries, where tuberculosis is endemic, it must always be considered in the differential diagnosis of many lesions. We report a rare case of tuberculosis of the tongue associated with lymph nodes localization.
Case Report
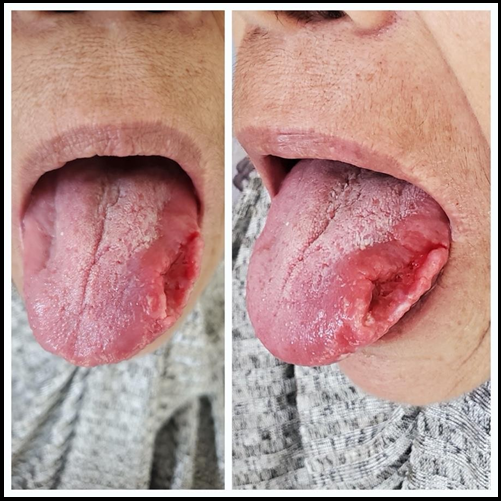
We present a case of a 65-year-old female patient, visited our department with the chief complaint of painful ulcer on the left lateral border of the tongue (Figure 1) developed 1 month ago without any apparent initiating event such as trauma or systemic illness. The patient’s medical history reported no personal history of TB or notion of TB contagion.
Intraoral examination revealed an ulcerated lesion measuring approximately 2.5 cm in diameter on the left lateral border of the tongue, tender with irregular border, bleeding on touch, the base of lesion was firm in consistency on digital palpation. The remaining part of the tongue was normal in texture and color. Mobility of tongue was normal and not deviated to either side on protrusion.
Extraoral examination revealed the presence of bilateral lymph node involvement. Based on the clinical examination, squamous cell carcinoma was suspected, therefore an incisional biopsy of the ulcer was carried out. Histological examination revealed the diagnosis of lingual TB.
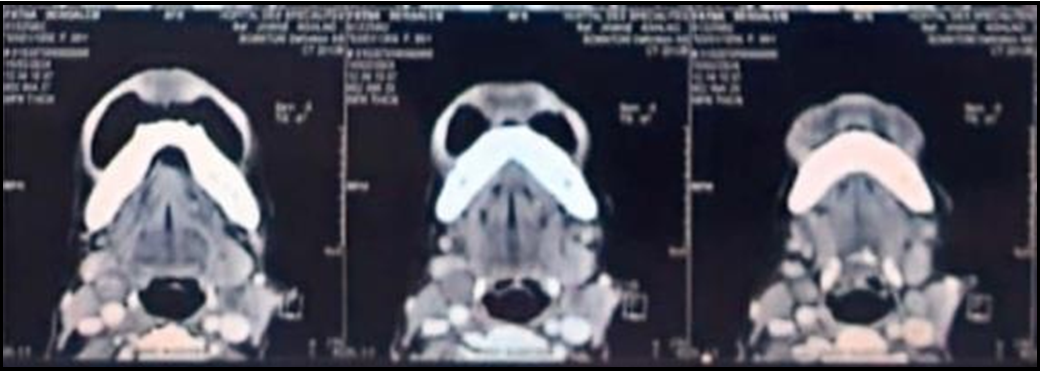
An additional workup including a cervicofacial and thoracic Ct scan was initiated to rule out pulmonary tuberculosis and to search for another localization; revealed the association of lymph node tuberculosis (Figure 2), a Phthisiology’s specialist’s opinion was sought to start antituberculosis treatment.
Figure 1: Images of the patient showing the ulcerated lesion of the left lateral border of the tongue.
Figure 2: Cervicofacial CT scan in axial section showing a necrotic bilateral cervical adenopathies.
Discussion
In its Global Tuberculosis Report for 2023, the World Health Organization (WHO) revealed alarming numbers for the tuberculosis situation in Morocco. The number of new cases and relapses recorded in the previous year was 30,503, bringing the total number of people infected with the disease in Morocco to around 35,000.
According to the WHO, this represents an incidence of 93 cases per 100,000 inhabitants.
Contagious and transmissible pulmonary tuberculosis accounts for around 53% of all cases of infection in Morocco [1].
In the cervicofacial region, tuberculosis most often affects the lymph nodes.
Localization in the buccal mucosa is very rare, clinical manifestations are non-specific.
The tongue is the most commonly affected site of oral TB; However, it can affect buccal gingiva, mucosa, palatine tonsil, lips, palate, floor of the mouth and the salivary glands [2].
Tuberculosis of the tongue may be either a primary or secondary occurrence. It’s quite a rare phenomenon in both cases, especially in primary form when it’s seen in younger patients often associated with enlarged cervical lymph nodes. The secondary form usually coexists with pulmonary disease and may occur in all age groups; however, middle-aged and older people are more likely involved, two routes of contamination are described: Direct inoculation (infected by sputum products through a small break in the surface) and hematogenous route (deposited in the submucosa, and subsequently to proliferate and ulcerate the overlying mucosa).
TB of the tongue may involve the tip or lateral margins as described in our case. Classically, The lesion is generally ulcerated painful, with irregular margins and an indurated, necrotic base covered by a yellowish coating [3]. However, it can be presented in a various form, such as ulcers, nodule, plaques, fissures, or vesicles, which mimics tongue cancer and also other various systemic diseases might cause a similar lesion, including Crohn’s disease, syphilis, blastomycosis infection, histopathological examination and culture of microorganisms should be considered for definite diagnosis [4].
Diagnosis is much more difficult in cases of primary tuberculosis. Additional examinations (anatomopathological examination of a sample, culture, PCR) will reveal the etiology of this ulceration and rule out squamous cell carcinoma. However, the low bacillary load in oral lesions may explain why the search for M.tb by culture or direct examination may give negative results [5]. Whether it is primary or secondary tuberculosis, the initiation of systemic anti-tuberculosis treatment is essential, Currently, the most effective regimens require a combination of 4 drugs [isoniazid (INH), rifampicin (RIF), pyrazinamide (PZA), and ethambutol (ETO)] administered daily for the first 2 months, followed by an additional 4 months with 3 drugs (INH, RIF and ethambutol). The treatment allow rapid improvement of ulceration and general condition; its efficacy has changed the previously unfavorable prognosis of this tuberculous localization.
Conclusion
Tuberculosis of the tongue, whether primary or secondary, is quite a rare phenomenon. It should be suspected in the presence of chronic ulceration and included in the differential diagnosis, confirmed by histopathological examination and culture for the presence of tubercle bacilli. Initiation of anti-tuberculosis treatment leads to rapid improvement in ulceration and general condition; its efficacy has changed the previously unfavorable prognosis of this tuberculous localization.
Conflicts Of Interest: No conflicts of interest have been declared by the authors.
References
- Plan stratégique national pour la prévention et le contrôle de la tuberculose au Maroc 2024-2030.
- Kapoor S, Gandhi S, Gandhi N, Singh I (2014) Oral manifestations of tuberculosis. Chrismed J Health Res. 1(1): 11– 4.
- Kakisi OK, Kechagia AS, Kakisis IK, Rafailidis PI, Falagas ME (2010) Tuberculosis of the oral cavity: a systematic review. Eur J Oral Sci. 118(2): 103–9.
- Facciolo MT, Riva F, Gallenzi P, Patini R, Gaglioti D (2017) A rare case of oral multisystem Langerhans cell histiocytosis. J Clin Exp Dent. 9(6): e820–e824.
- Gupta PP, Fotedar S, Agarwal D, Sansawal P (2007) Primary tuberculous glossitis in an immunocompétent patient. Hong Kong J Med. 13(4): 330-1.